High Levels of ‘Bad’ Cholesterol Linked to Increased Risk of Early-onset Alzheimer’s, Study Suggests
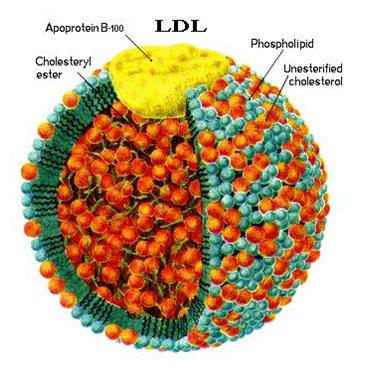
High levels of “bad” cholesterol, known as low-density lipoprotein (LDL), might increase the risk of developing early-onset Alzheimer’s disease, a study suggests.
The study, “Association of Early-Onset Alzheimer Disease With Elevated Low-density Lipoprotein Cholesterol Levels and Rare Genetic Coding Variants of APOB,” was published in the journal JAMA Neurology.
Early-onset Alzheimer’s, when people develop symptoms before age 65, is a rare form of the disease, accounting for 10% of cases.
Research has shown that mutations in certain genes — amyloid precursor protein (APP), presenilin 1 (PSEN1), and presenilin 2 (PSEN2) — may cause early forms of Alzheimer’s. However, these mutations are found in only 10% of cases, and researchers still do not know the underlying cause for the other 90%.
High cholesterol levels have been linked to late-onset Alzheimer’s, the most common form of the disease. In fact, the well-known genetic variant APOE E4, which increases the risk of late-onset Alzheimer’s, causes a rise in LDL cholesterol.
LDL is sometimes called the “bad” cholesterol because high LDL levels lead to a buildup of cholesterol in the arteries. Medicines used to lower cholesterol levels have been shown to decrease the risk of Alzheimer’s.
However, the role of cholesterol in early-onset Alzheimer’s and whether genetic variants might contribute to a possible link between the two remain unknown.
To address this, researchers at the Atlanta Veterans Affairs (VA) Medical Center and Emory University explored how cholesterol and its genetic basis might be associated with early-onset Alzheimer’s.
“The big question is whether there is a causal link between cholesterol levels in the blood and Alzheimer’s disease risk,” Thomas Wingo, the study’s lead author, said in a press release. Wingo is a neurologist at the Atlanta VA and the Emory University School of Medicine.
They analyzed the DNA for common Alzheimer’s-causing mutations — APP, PSEN1, PSEN2, and APOE E4 — in 654 patients with early-onset Alzheimer’s (mean age 55.6 years) and 1,471 individuals used as controls (mean age 72 years).
While the analysis showed that APOE E4 was closely related to early disease, the genetic variant only explained roughly 10% of the cases, a ratio similar to that seen in late-onset Alzheimer’s. At least one of the other genes linked to Alzheimer’s was found in 3% of early cases.
Next, the researchers analyzed cholesterol levels in 267 patients with early-onset Alzheimer’s and found that after controlling for APOE E4, early-onset cases had higher levels of total cholesterol and LDL cholesterol than controls: 131.6 mg/dL versus 104.4 mg/dL, respectively.
These results suggest that levels of LDL could be an independent risk factor for early-onset Alzheimer’s, regardless of whether people have the APOE E4 gene variant.
“The existing data have been murky on this point. One interpretation of our current data is that LDL cholesterol does play a causal role. If that is the case, we might need to revise targets for LDC cholesterol to help reduce Alzheimer’s risk. Our work now is focused on testing whether there is a causal link,” Wingo said.
They found no correlation between high-density lipoprotein (HDL) cholesterol levels — the “good” cholesterol — and early-onset disease.
The researchers also found a new potential genetic risk factor for early-onset Alzheimer’s. APOB, a protein responsible for the metabolism of fats (lipids), including cholesterol, had been previously linked to the disease. When the team looked for genetic variations of the APOB gene, it found that 5% of early-onset cases carried a genetic variant of this gene, compared with only 1.7% of the controls.
One particular APOB gene variation — called p154R>X — was associated with very low levels of LDL, meaning that some variants of this gene could have a protective effect.
Nonetheless, neither APOE nor APOB could entirely explain the elevated levels of LDL in early-onset Alzheimer’s patients, suggesting that other genes and molecular mechanisms play a role in cholesterol and Alzheimer’s risk.
“Our study provides evidence that circulating cholesterol is associated with [early-onset Alzheimer’s disease] independently of APOE E4. Furthermore, we have identified novel rare genetic coding changes in APOB that are associated with [early-onset Alzheimer’s] independently of APOE,” the researchers concluded.






